Effect of Enteral Glutamine Supplementation in
Critically Ill Patients: A Systematic
Review and Meta-Analysis
Li-Mei Lin1, Li-Wei Chen2,3, Chia-Ying Lo1
1Department of Pharmacy, Keelung Chang Gung
Memorial Hospital;
2Department of Chinese Herbal Pharmacy, Taoyuan
Chang Gung Memorial Hospital;
3Department of Cosmetic Science, College of
Human Ecology,
Chang Gung University of Science and Technology
Abstract
Background: The suitability of glutamine supplementation to critically ill patients remains unclear. In this systematic review, we aimed to assess the effect of enteral glutamine supplementation on mortality, infection, and length of stay (LOS) in critically ill patients.
Methods: We searched for randomized trials involving critically ill patients who received enteral administered glutamine in the CENTRAL, MEDLINE, EMBASE, CINAHL, Science Citation Index, and Lilacs databases. The primary outcome was all-cause mortality.
Results: Of the 880 patients from the 10 included trials, 439 (49.9%) received enteral glutamine (GLN group) and 441 (50.1%) received routine standard care or no treatment (control group). Six studies reported mortality values, and 6 provided the incidence of infection. Enteral glutamine treatment did not significantly reduce the risk of all-cause mortality (relative risk [RR], 0.94; 95% confidence interval [CI], 0.65–1.36; p = 0.24; I2 = 26%) and infectious complications (RR, 0.85; 95% CI, 0.63–1.16; p = 0.07; I2 = 50%). However, the LOS was shorter in the GLN group than in the control group (mean difference [MD], -7.54 days; 95% CI, -13.17 to -1.92; p =0.10; I² = 48%).
Conclusion: Enteral glutamine supplementation in critically ill patients does not offer the benefits of reducing mortality and infectious morbidity, although it may decrease the LOS.
Keyword: glutamine, critically ill patient, mortality, infection, length of stay
Background
Glutamine—a 5-carbon amino acid—is the most abundant amino acid in the body, and was proposed as a conditional amino acid by Lacey and Wilmore in 1990. Glutamine serves as a major fuel source, regulates DNA and RNA synthesis in mucosal cells and immune system cells, and maintains several other important functions in human metabolism. Glutamine is increasingly utilized by proliferating lymphocytes and immune-stimulated macrophages during critical illnesses. Lacey et al demonstrated that patients with low plasma and tissue levels of glutamine had poor clinical outcomes1. Some studies indicated that glutamine supplementation may reduce the mortality, infectious morbidity, and hospital length of stay (LOS)2. In contrast, several recent randomized controlled trials indicated that glutamine supplementation in critically ill patients had no benefits3.
In the present study, we aimed to systematically review and synthesize randomized clinical trial data to assess the effects of enteral glutamine supplementation, in comparison with other treatment methods, on the clinical outcomes of critically ill patients.
Methods
Literature search
Three authors (LML, CYL, and LWC) independently performed a search of the following databases: CENTRAL (The Cochrane Library, latest issue), MEDLINE (January 1950 to March 2016), EMBASE (January 1980 to March 2016), CINAHL (January 1982 to March 2016), and the Science Citation Index (January 1981 to March 2016). There was no language restriction to identify the relevant studies. We conducted a combined exploration of the Medical Subject Headings (MeSH) with a truncation tool, and applied the filter method to isolate randomized controlled trials, as described in the Cochrane Handbook for Systematic Reviews of Interventions (http://www.cochranehandbook.org). We conducted the search using the following key words: glutamine, dipeptide, L-glutamine, immunonutri*, and immunoenhanc* (The asterisk symbol represents that a truncation search feature provides the ability to search for variant words or spellings.). To expand our search, we also hand-searched reference lists of the potentially related articles.
Study selection
All the authors independently screened the relevant trials identified by the literature search. We included all the randomized trials involving critically ill patients aged ≥18 years who received enteral glutamine supplementation in addition to routine standard care. Participants who were admitted to the intensive care unit (ICU) with major surgery, burns, trauma, acute pancreatitis, or other severe medical illness were included. The studies with control groups that did not receive any nutrient supplementation were also included. We excluded studies on neonates and pediatric patients. Studies of adults undergoing bone marrow transplantation or chemotherapy were also excluded.
Data extraction and quality assessment
Two investigators (LML and CYL) independently extracted the data and assessed trial quality. We consulted a third author (LWC) in cases of disagreement and for quality assurance of the processes. We screened the abstracts and potential manuscripts for data extraction. A pre-designed standard form was used to extract the following information: characteristics of the study (study settings, designs, methods of randomization), participants, interventions, and outcomes (types of outcome measures, timing of outcomes, adverse events). Our primary outcome of interest was all-cause mortality (hospital or ICU). The secondary outcomes included infectious complications and LOS in the hospital or ICU. If the 28-day mortality rate was not reported, we used the hospital mortality rate in those cases.
Moreover, we used the methodological quality assessment described by Heyland et al4 to evaluate trial quality. The methodological quality assessment is a scoring system containing 9 parameters to estimate study quality. Based on this scoring system, we defined a higher methodological score as a score of ≥8 (range, 0–14).
Data synthesis and statistical analysis
We performed data synthesis and statistical analyses using RevMan 5.3. We collected dichotomous outcomes from individual studies to compute the relative risks (RRs) with 95% confidence intervals (CIs), and to estimate the pooled Mantel-Haenszel (M-H) RR and calculate the associated 95% CI. We used the random effects model (DerSimonian-Laird method) to estimate the overall RR due to the pragmatic distributional treatment effects. For continuous outcomes, the mean difference (MD) with corresponding 95% CI was used. The heterogeneity was assessed using the I2 statistic (I2 ≥ 50% indicated a substantial level of heterogeneity), as well as the Q-statistic with its degrees of freedom (df).
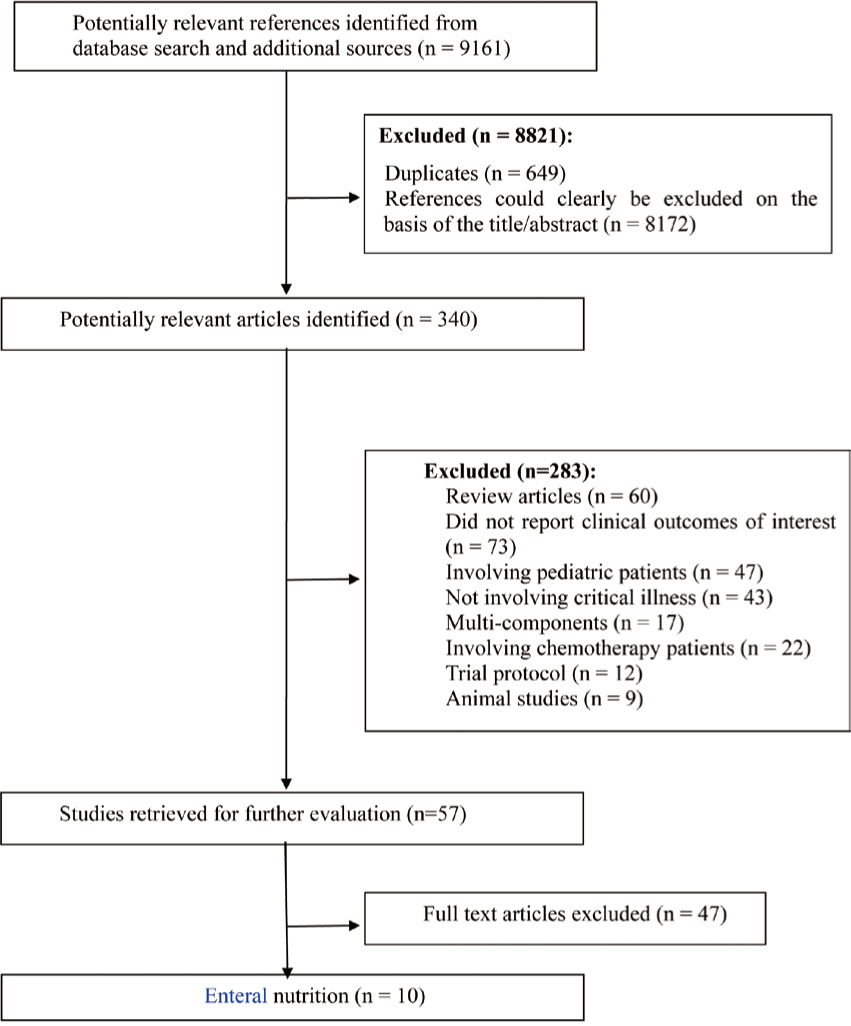
Figure 1. Flow diagram of trial inclusion.
Table 1. Key characteristics of the included trials (oral glutamine supplementation)
Figure 2. Forest plot of the effect of enteral glutamine supplementation on mortality
Figure 3. Forest plot of the effect of enteral glutamine supplementation on infection rate
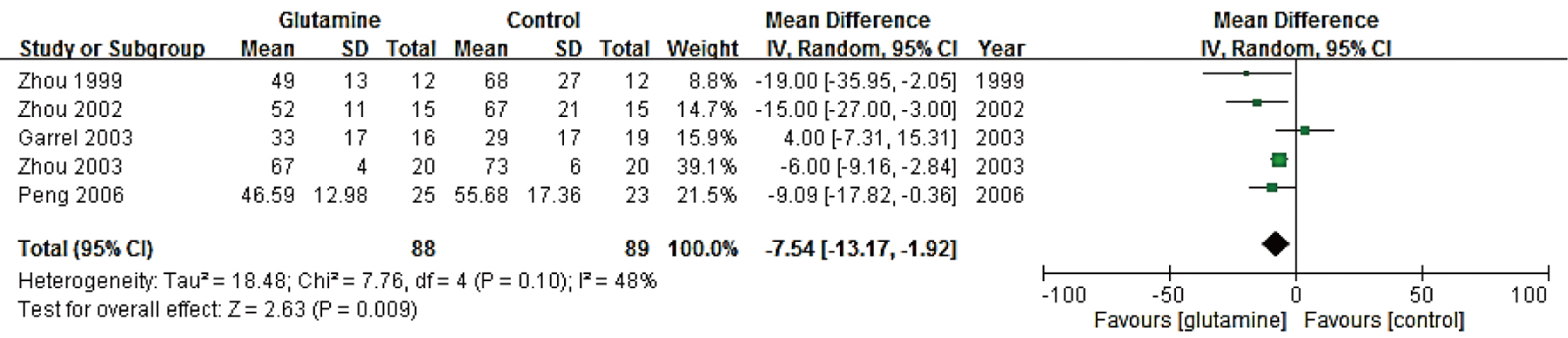
Figure 4. Forest plot of the effect of enteral glutamine supplementation on hospital length of stay
Results
Figure 1 provides a summary of the literature search and selection process. A total of 9161citations were identified during the initial study retrieval process. After screening the titles and abstracts of potential references, we excluded 8821 citations. After reading the full text of the articles, a total of 10 randomized trials involving 880 patients that compared oral nutrition with other care methods were found to meet the inclusion criteria. The characteristics of the included enteral glutamine trials are presented in Table 1. Since there was no language restriction, we included 2 articles in Chinese as well. Of these studies, 5 enrolled burn patients, and another 5 trials included medical patients, traumatic patients, burn patients, surgical patients, and patients with pancreatitis.
Impact on mortality
Six trials involving 778 patients reported hospital or ICU mortality data. The data were combined to evaluate the overall effect of enteral glutamine supplementation on mortality. No heterogeneity among these studies was observed (I2 = 26%, p = 0.24). Enteral glutamine supplementation had no effect on overall mortality (M-H RR, 0.94; 95% CI, 0.65–1.36; Figure 2).
Impact on the infection rate
A total of six trials involving 728 patients were assessed to estimate the effect of GLN supplementation on the infection rate. The incidence rate was 32.87% in GLN group and 36.08% in control group. Pooled analysis of these trials indicated no benefit (M-H RR, 0.85; 95% CI, 0.63–1.16; Figure 3).
Impact on hospital stay
Only 5 trials (177 participants) reported on the hospital or ICU LOS, and these values were combined to estimate the effect of GLN supplementation on the LOS. Enteral glutamine supplementation significantly decreased the LOS (weighted MD, -7.54; 95% CI, -13.17 to -1.92; Figure 4). The test for heterogeneity indicated significant results (I2 = 48%).
Discussion
The results of the meta-analysis indicated that enteral glutamine supplementation has no effect on reducing the mortality and infectious morbidity in critically ill patients. Nevertheless, enteral glutamine supplementation can reduce the hospital LOS. Moreover, the qualities of the clinical trials included in our study were mostly moderate. Hence, the efficacy of glutamine supplementation for critical ill patients should be confirmed by studies with a higher quality.
According to the characteristics of critically ill patients involved in the trials, most of recipients were burn. Of these 10 trials, 5 included burn patients. The European Society for Clinical Nutrition and Metabolism (ESPEN) guideline recommends (1) In patients with burns > 20% body surface area, additional enteral doses of GLN (0.3-0.5g/kg/d) should be administered for 10-15 days as soon as EN is commenced. (2) In ICU patients except burn and trauma patients, additional enteral GLN should not be administered5. Hence, future studies should aim to clarify the benefits of enteral glutamine supplementation in patients with different severe conditions.
This study has certain limitations. The first limitation concerns the variation in the study quality. The second limitation is rooted in the reporting of LOS, which varied in median and range. Moreover, there was moderate to substantial heterogeneity within the included studies in our analysis.
Conclusion
In conclusion, our findings did not definitely confirm that enteral glutamine supplementation should be administered in critically ill patients. Furthermore, it is very important to conduct additional powered randomized controlled trials.
List of abbreviations
LOS, length of stay; GLN, glutamine; RR, relative risk; CI, confidence interval; M-H, Mantel-Haenszel ; MD, mean difference; ICU, intensive care unit
Acknowledgments
We thank the support of CMRPG2B0431 from Chang Gung Memorial Hospital, Keelung, Taiwan. The authors bear all responsibility and have no conflict of interest with regard to this work.
References:
1. Lacey JM, Wilmore DW: Is glutamine a conditionally essential amino acid? Nutr Rev 1990;48:297-309.
2. Oliveira GP, Dias CM, Pelosi P, et al: Understanding the mechanisms of glutamine action in critically ill patients. An Acad Bras Ciênc 2010;82:417-30.
3. Andrews PJ, Avenell A, Noble DW, et al: Randomised trial of glutamine, selenium, or both, to supplement parenteral nutrition for critically ill patients. BMJ 2011;342:d1542.
4. Heyland DK, Novak F, Drover JW, et al: Should immunonutrition become routine in critically ill patients? JAMA 2001;286:944-53.
5. Singer P, Blaser AR, Berger MM, et al. ESPEN guideline on clinical nutrition in the intensive care unit. Clin Nutr 2019;38(1):48-79.
6. Jones C, Palmer TE, Griffiths RD: Randomized clinical outcome study of critically ill patients given glutamine-supplemented enteral nutrition. Nutrition 1999 ;15(2):108-15.
7. Zhou Y, Jiang Z, Sun Y: Glutamine dipeptide enriched enteral nutrition improving gut permeability in severe burns. Zhonghua Yi Xue Za Zhi 1999;79(11):825-7.
8. Conejero R, Bonet A, Grau T, et al: Effect of a glutamine-enriched enteral diet on intestinal permeability and infectious morbidity at 28 days in critically ill patients with systemic inflammatory response syndrome: a randomized, single-blind, prospective, multicenter study. Nutrition 2002;18(9):716-21.
9. Zhou Y, Sun Y, Jiang Z, et al: The effects of glutamine dipeptide on the improvement of endotoxemia in severely burned patients. Zhonghua Shao Shang Za Zhi 2002;18(6):343-5.
10. Garrel D, Patenaude J, Nedelec B, et al: Decreased mortality and infectious morbidity in adult burn patients given enteral glutamine supplements: a prospective, controlled, randomized clinical trial. Crit Care Med 2003;31(10):2444-9.
11. Hall JC, Dobb G, Hall J, et al: A prospective randomized trial of enteral glutamine in critical illness. Intensive Care Med 2003;29(10):1710-6.
12. Zhou Y, Jiang Z, Sun Y, et al: The effect of supplemental enteral glutamine on plasma levels, gut function, and outcome in severe burns: a randomized, double-blind, controlled clinical trial. JPEN J Parenter Enteral Nutr 2003;27(4):241-5.
13. Peng X, Yan H, You Z, et al: Glutamine granule-supplemented enteral nutrition maintains immunological function in severely burned patients. Burns 2006;32(5):589-93.
14. Kumar S, Kumar R, Sharma SB, et al: Effect of oral glutamine administration on oxidative stress, morbidity and mortality in critically ill surgical patients. Indian J Gastroenterol 2007;26(2):70-3.
15. Singh N, Mishra SK, Sachdev V, et al: Effect of oral glutamine supplementation on gut permeability and endotoxemia in patients with severe acute pancreatitis: a randomized controlled trial. Pancreas 2014 ;43(6):867-73.
重症病人腸道補充麩醯胺之效益:
系統性回顧與統合分析
林麗梅1、陳立偉2,3、羅嘉盈1
1長庚醫療財團法人基隆長庚紀念醫院藥劑科
2長庚醫療財團法人桃園長庚紀念醫院中醫藥劑部
3長庚科技大學民生學院化妝品應用系
摘要
背景:重症病人補充麩醯胺(glutamine)的適當性目前仍無定論,本研究的主要目的為評估重症病人腸道補充麩醯胺之死亡率、感染率及住院天數的效益分析。
方法:以腸道補充麩醯胺之重症病人為研究對象,在CENTRAL、 MEDLINE、 EMBASE、 CINAHL、 Science Citation Index和Lilacs等資料庫搜尋隨機對照試驗的文獻,並將任何原因導致病人的死亡率,定義為本研究的主要結果。
結果:共計10個試驗與880位病人納入分析,分別有439位 (49.9%)腸道補充麩醯胺(為GLN組),及441位 (50.1%)接受常規標準治療且未額外給予營養治療 (為對照組)。其中有6個研究呈現死亡率數值,及6個研究分析兩組病人的感染率。
本研究分析結果:腸道補充麩醯胺未顯著降低死亡率 (相對風險為0.94,95%信賴區間為0.65至1.36,p值為0.24,I2為26%)及感染率(相對風險為0.85,95%信賴區間為0.63至1.16,p值為0.07,I2為50%);但是腸道補充麩醯胺可以減少住院天數 (平均差為-7.54天,95%信賴區間為-13.17至-1.92,p值為0.10,I2為48%)。
結論:重症病人腸道補充麩醯胺不能降低死亡率及感染率,但是能夠減少此類病人的住院天數。
通訊作者:林麗梅/通訊地址:基隆市麥金路222號
服務單位:長庚醫療財團法人基隆長庚紀念醫院藥劑科/聯絡電話:(O) 02-24313131
ext 2098